Achilles Insertional Debridement (Spur Removal) & Repair
Achilles tendon problems at the back of the heel (insertion) are usually degenerative in nature and result in pain and a bony prominence. The medical term is ‘insertional achilles tendinopathy’. The first line therapy includes physiotherapy, accommodative footwear (heel raise, soft counter) and judicious use of anti-inflammatory medication and corticosteroid injections. If non-operative treatment fails, surgery can be helpful. The most commonly used procedure is debridement of the tendon, resection of the prominent bone and repair of the tendon.
The Surgery
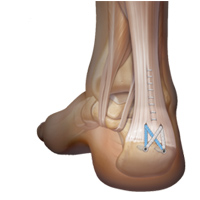
You will need to have a general anaesthetic and local anaesthetic. Antibiotics are administered intra-venously. You are then carefully positioned on the surgical table so as to allow access to the back of the heel. At the site of the prominence, a longitudinal incision is made and the tendon insertion is exposed. The tendon is removed off the heel bone and trimmed of degenerate tissue. The prominent bone at the back of the heel bone is removed. The tendon is then re-attached to the heel bone with strong plastic anchors. The skin is carefully closed and a cast is applied.
Post-Operatively
You will have your foot elevated on 1-2 pillows to reduce swelling. The local anaesthetic should provide you with pain relief, and may make your foot and toes temporarily numb. You will generally spend the night in hospital and you will be safe to ambulate with crutches, as soon as you feel comfortable. You will need to take medications for pain relief and for DVT prevention (injections or Aspirin). The cast and sutures are removed at 2 weeks and you will be placed into a CAM boot. You will need to see a physiotherapist for rehabilitation. Below is an estimate of your recovery.
- Activity
- Timeframe (approximate)
- No weight bearing in cast
- 0-2 wks
- Walking with boot with crutches
- 2wks - 6wks
- Physiotherapy
- 6wks -
- Full Recovery
- 6 -12 mts
- Type of Activity
- Time-frame
- Walking
- 2 weeks
- Driving (right ankle)
- 8 weeks
- Jogging
- 4-6 months
- Sport
- 6-12 months
Risks of surgery
All surgical procedures carry some risk. The risk of complications with Achilles rupture repair is low. Most patients benefit from this surgery. A small number of patients are not better or can be made worse. You should weigh up the benefits with the risks prior to electing to have surgery.
This is a list of the most common problems which can/do occur
- Infection – minimised with antibiotics, elevation, keeping the dressing clean and dry
- Nerve injury – resulting in numbness or pins and needles, occasionally pain
- Wound healing problems – increased if smoking, diabetes, poor circulation
- Stiffness – reduced range of movement of the ankle joint
- Swelling – is normal and improves with time
- Bleeding – usually minimal and visible in dressing
- Pain – which may require stronger medication
- Recurrence – the tendon may remain painful or re-tear and you may need further surgery
- DVT – clot/s in the deep veins of the leg (increased if smoking, contraceptive pill, hormone replacement or previous DVT)
- PE – pulmonary embolus, or DVT clots that travel to the lung resulting in breathing problems
- Complex regional pain syndrome (CRPS) – nerve pain syndrome, risk reduced with Vitamin C 500mg daily for 40 days
- Anaesthetic complications – more likely if there are pre-existing medical disorders
You will need the Adobe Reader to view and print these documents.
![]()









